Blog
Life during lockdown in England: charting the impact on young people's mental health
The Covid-19 pandemic is affecting lives around the globe. Miriam Sorgenfrei explains how the latest adolescent mental health data suggests that some groups have been affected more than others, and that many young people have been unable to access effective early intervention support.
The Mental Health of Children and Young People in England (MHCYP) 2020 survey was conducted for the NHS in July and August 2020. The survey involved a representative sample of 3,570 children and young people, including 1,308 11–16-year-olds. The data provides insights into the probable prevalence of mental disorders in adolescents.
 The survey utilised the Strengths and Difficulties Questionnaire (SDQ) to assess respondents’ mental health. This measure provides an indication of respondents’ mental health status but cannot diagnose any disorders. An independent study, however, has shown that 81–91% of young people identified as having a probable mental disorder using the SDQ met the criteria for a clinical diagnosis, which suggests that this measure, while it is not diagnostic, is a good indication of young people’s mental health.
The survey utilised the Strengths and Difficulties Questionnaire (SDQ) to assess respondents’ mental health. This measure provides an indication of respondents’ mental health status but cannot diagnose any disorders. An independent study, however, has shown that 81–91% of young people identified as having a probable mental disorder using the SDQ met the criteria for a clinical diagnosis, which suggests that this measure, while it is not diagnostic, is a good indication of young people’s mental health.
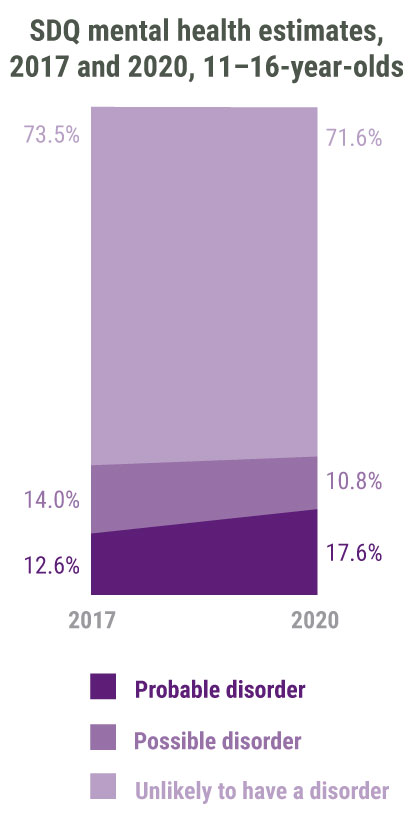
A disorder is considered probably present if scores on the relevant symptoms (emotional, behaviour and hyperactivity) of the SDQ indicate a young person is above the 95th percentile. A disorder was considered possible with intermediate scores on SDQ.
According to this latest data from the MHCYP, the proportion of young people with a probable mental disorder has increased by five percentage points since the previous 2017 survey. Due to the nature of the data, it isn’t possible to quantify how many individual assessment results were different from the previous round (i.e. we don’t know how many young people who had a probable mental disorder in 2017 received help and are now unlikely to have a mental disorder and vice versa). Nevertheless, it’s evident that, overall, the extent of mental health difficulties hasn’t increased as much as the average severity of reported symptoms.
Young people aged 11 to 16 had 1.4 times higher odds of having a probable mental disorder in 2020 compared with those in 2017, and 1.3 times lower odds of having a possible disorder. One conceivable interpretation of the latest figures is that many of those who would – under different circumstances – have a possible mental disorder, instead experienced additional stress or adversity, and thus have a probable mental disorder. Increased symptom severity might be linked to the Covid-19 pandemic: young people are having to cope with a new, stressful and uncertain situation while struggling to access appropriate early intervention support.
The latest data highlights the urgency of making evidence-based early intervention available.
- Mental health promotion interventions are needed to enhance young people’s wellbeing and resilience. It’s interesting that the proportion of youth unlikely to have a mental disorder has not changed much despite the lockdown measures in place. Providing all young people with access to interventions that enhance wellbeing and strengthen protective factors is essential to prevent future difficulties.
- Interventions designed to prevent the onset of mental health problems by targeting risk factors are equally needed. The proportion of those with a possible mental disorder has decreased while the proportion of those with a probable mental disorder has increased. Interventions that aim to reduce mental health difficulties are essential to protect those with possible or probable mental disorders and prevent their symptoms from worsening.
Alarmingly, the proportion of those with a probable mental disorder has increased, suggesting there is insufficient effective targeted support available.
Life during lockdown
The latest MHCYP survey examined young people’s circumstances during lockdown, including, for example, their engagement in extra-curricular activities, and the impact of the lockdown on their household’s financial circumstances, access to home learning facilities and perceived anxiety levels. Changes made to young people’s lives during lockdown and the perceived impact of these changes varied, with those with probable mental disorders reporting more extensive impact on their lives than those who are unlikely to have mental disorders. Making targeted and comprehensive help available and accessible is crucial to enhance adolescent wellbeing and mitigate disadvantages.
Overall perceived impact
The MHCYP asked young people whether life in lockdown had been ‘much better’, ‘a little better’, ‘neither better nor worse’, ‘a little worse’ or ‘much worse’. Those with probable disorders were 5.6 times more likely to say that life is ‘much worse’ than those who are unlikely to have a mental disorder.
Activities during lockdown
There were substantial differences in how active youths with and without probable mental disorders were during the lockdown. Those with probable mental disorders were less likely to engage in exercise, either outdoors or indoors, to meet friends outside, read a book, cook, bake, do crafts, call or video-call friends or relatives, eat or spend time with the family, or do schoolwork.
The probability of having a mental disorder also correlated with increased anxiety levels. Young people aged 11 to 16 with probable mental disorders scored higher on all subscales of the Pandemic Anxiety Scale than those with possible disorders and those who are unlikely to have any disorders.
Accessing mental health support
Nearly one in five (18.9%) young people with a probable mental disorder tried to seek help but did not receive the help they sought. While around half (51.8%) of those with probable mental disorders did not have any contact with mental health services, only one in nine (11.2%) received help from services as normal. One in 10 (10.7%) said sessions were cancelled, and one in five (19.4%) had an appointment or treatment session changed from face-to-face to virtual delivery. Note that respondents could select more than one of these options, which is why the total does not equal 100%.
Early intervention needs to be made available and accessible to all
One of the UN's sustainable development goals, specifically number three, is to ensure healthy lives and promote wellbeing for all at all ages. The latest representative data on adolescent mental health not only shows an alarming increase in symptom severity, which might be preventable through effective early intervention, but also reveals that one in five of those with a probable mental disorder who actively sought help, did not receive any support.
Mental health support must be made available to all adolescents in the UK. Evidence-based mental health interventions, which have been proven to strengthen young people’s mental health and wellbeing and prevent the development of disorders, play an essential role in mitigating the impact of adversities such as Covid-19 and lockdown restrictions.
Effective interventions that are designed to reduce depression and anxiety symptoms need to be accessible to those needing or wanting support. Ensuring that those who seek support receive it’s the bare minimum, but efforts also need to be made to reach those at risk of developing symptoms. One of the challenges resulting from Covid-19 is finding new ways to identify families or young people who need additional support.
Evidence-based interventions at the universal and targeted levels need to be offered widely and prospective participants need to be actively recruited to ensure young people’s wellbeing. Digitally delivered interventions have the potential to make appropriate support available to a broader audience, but any changes made to evidence-based face-to-face support services need to be carefully planned and evaluated, keeping in mind the challenges and risks to moving to virtual delivery.
Schools also play an important role in supporting young people’s mental health. To better understand which school-based interventions improve adolescent mental health and under what circumstances programmes are effective, we are currently undertaking an evidence review. Results will be available in spring 2021.
